Dementia is a common name for a series of symptoms that lead to the loss of mental abilities, such as the ability to think, remember, and reason logically, as well as changes in behavior, character, and unexpected changes in mood.
Dementia significantly impairs the quality of life. Finding out that you have this disease can be very uncomfortable at first, but there are more and more ways to make the life of people with dementia as high quality as possible. Caring for such patients is physically and emotionally exhausting, time-consuming and economically exhausting, so it can seriously affect the psychophysical health of the caregiver and the family. Insight into the growing number of available assistance measures facilitates the process of dementia care and somewhat maintains the level of quality of general functioning.
The most common questions that arise regarding this increasingly widespread health problem:
- What is dementia?
- Are there early warning signs?
- How to accept the new condition and prepare for the changes that inevitably come in the further course of the disease?
What is dementia?
There are a number of conditions that fall under the general label of dementia. The most common is Alzheimer’s disease, which affects 50 to 70% of dementia patients. Different dementias affect the brain’s ability to think and remember, dramatically affecting a person’s ability to perform everyday tasks. In its advanced forms, dementia patients cannot survive without constant care.
To a greater or lesser degree, there are changes in memory, planning, decision-making, spatial orientation, speech, and mood. The onset of the disease is usually gradual, the symptoms at the beginning can be so mild that they are hardly noticeable. Deterioration is usually slow, but inevitably leads to behavior disorders and personality changes, and to the complete loss of everyday skills, i.e. to the point that the affected person ceases to be independent, and in the advanced stage cannot dress, bathe, eat, or walk independently.
Types of dementia
After Alzheimer’s disease, the next most common form of dementia is vascular dementia. This condition can occur after a stroke and accounts for about a quarter of dementia cases. Other relatively common forms include dementia with Lewy bodies and frontotemporal dementia.
Alzheimer’s dementia
This is the most common type of dementia – around two-thirds of people with dementia have Alzheimer’s disease. Although we still do not know the definitive causes, it is known that typical changes occur in the brain – a decrease in brain volume and impairment of brain functions.
The disease goes through three stages. In the early stage, there are noticeable problems in remembering new events, orientation in space, even in a familiar environment. There may also be problems in managing finances (e.g. paying bills). There may also be difficulties in terms of speech, in terms of understanding more complex sentences, and finding words. Independence is only slightly impaired and patients can function with less intervention from the outside and most often live in their own household. Depression, apathy and anxiety sometimes occur. In the second, so-called in the moderate or middle stage of the disease, there is a deterioration of the already mentioned cognitive functions, which leads to a significant impairment of activities in everyday life. At this stage, there is a risk of manifesting more pronounced disorders in terms of behavior and psychological problems that worsen the already significantly damaged independence of the patient and there is a state when they cannot go out of their house alone and/or live without another person. In the third phase, the so-called in the late stage of the disease, which implies almost complete dependence on another person, patients have problems with basic simple activities, such as eating, bathing and dressing.
As the disease progresses, patients seem to forget to walk and are increasingly mobile, to the stage where they become bedridden. The slowness and stiffness that develops may resemble Parkinsonism. Epileptic seizures can also occur at this stage. All this leads to a high risk of developing pneumonia, urinary infections and other conditions that can end fatally.
Frontotemporal dementia
Frontotemporal dementia is a group of conditions that affect the frontal and/or temporal lobes of the brain. If the frontal lobes are more affected, there will be more pronounced difficulties with motivation, planning and organizing, controlling emotions and maintaining socially acceptable behavior. In the case when the temporal lobes are affected, difficulties with speaking and/or understanding language are more pronounced. This dementia is more likely to affect younger people, most often occurring between the ages of 45 and 60.
Dementia with Lewy bodies
In this type of dementia, there are disturbances in motor activities (a picture reminiscent of Parkinsonism) with changes in attention and visual functions, as well as behavior, with the important thing being that mobility disorders and dementia develop in parallel or consecutively over several years. The state of consciousness and attention of the patients is variable from hour to hour or less, from episodes with severe confusion to almost normal functioning. Hallucinations, most often visual (images that other people do not see), occur very early in the onset of illness. For example, patients describe in detail images of animals, people or objects, scenes that others do not see. Unlike hallucinations in psychiatric diseases, fear and anxiety rarely occur here, so they are often not mentioned and should be asked specifically during the diagnostic interview. It is interesting to note that there are sleep disorders with “vivid dreams”, in which someone most often chases them, persecutes them and where, defending themselves, they can cause various injuries to themselves and the people around them. This disease is associated with the existence of “Lewy bodies” (specific protein clusters) in brain cells and their extensions.
Vascular dementia
This type of dementia can appear very quickly after a stroke (3 months) or develop gradually when it involves multiple changes in the small blood vessels of the brain. In this dementia, there are behavioral outbursts, as well as problems with attention, memory and speech. Unlike Alzheimer’s disease, here we can already expect motor symptoms, such as (most often) “Parkinsonism of the lower part of the body”. Progressive worsening in stages is common for this type of dementia.
Are there early warning signs?
Early signs of dementia can be subtle and difficult to recognize. They appear in different spheres of psychological life and general functioning.
These are some of the warning signs, if you answer “YES” to several of them, you should seek medical help.
- Are you having trouble recalling a recent conversation? Short-term memory loss can be an early symptom of dementia.
- Do you have difficulties in performing daily activities that were not a problem for you before, such as dressing, using household appliances, personal hygiene, making phone calls, etc.?
- Do you ever get lost in a familiar space? Do you have problems finding your way around public transport, difficulty finding your house or friend, post office, bank or a health center, despite having used that road for years. Does it happen that you can’t remember what day, month, year it is today?
- Do you have trouble planning – do you have trouble paying the bill, shopping at the grocery store without a list, packing lunch without a recipe?
- Speech problems – Forgetting certain words?
- Sudden mood swings – do you suddenly become sad and/or happy for no particular reason?
- Loss of motivation – Have you stopped doing activities that you used to like?
- Changes in sleep order – Do you sleep more than before, or do you sleep more during the day?
How to accept the new condition and prepare for the inevitable changes in the further course of the disease?
If you think you have dementia, it is important to see a doctor so that an accurate diagnosis can be made as soon as possible. Diagnostic procedures include a general examination, discussion of previous illnesses, discussion with the family/person who knows the patient, laboratory analyses, determination of thyroid hormone levels, determination of vitamin B12 levels, examination by a psychiatrist, neurologist, psychological and neuropsychological testing, brain imaging (CT or NMR ). A detailed full medical diagnosis and evaluation rule out treatable conditions such as vitamin B12 deficiency, thyroid disease, cardiovascular disease, cerebrovascular disease and chronic brain infections.
Early diagnosis enables the timely introduction of drugs that are available in our country and which are considered to delay the worsening of the symptoms of the disease. It also enables timely planning for the future, making financial and legal plans, access to appropriate services and support.
When the diagnosis is made, the patient and the caregiver or companion should receive information about the type of dementia, the further course and prognosis of the disease, the drugs the patient should take, the benefits and side effects of the treatment, as well as information about the attitude towards the patient. A doctor should explain things to you so that you understand them, answer questions, give advice and support, and listen.
Treatment of dementia
In the therapy of Alzheimer’s disease, drugs from two large groups are used, the so-called cholinesterase inhibitors (donepezil, rivastigmine, galantamine) and NMDA receptor antagonists (memantine), which are registered in our country. It is important to know that none of the drugs used lead to a cure for dementia. In the course of the disease, drugs used for various psychiatric symptoms such as depression, apathy, hallucinations, aggression, etc., such as anxiolytics, antidepressants and antipsychotics, will be needed.
Practical recommendations for patients
A diagnosis of dementia will likely mean that you will need to make changes in your daily life. You need to keep in mind that it is a progressive disease, which means that the patients become more and more dependent on another person and cannot live and function independently. This does not mean that big changes are needed immediately, but it is good to plan preparations for possible new situations in the further course of the disease. It would be a good idea to choose a trusted person yourself to handle your finances. In the same way, you should express your wish about the way of care in situations where you will need someone else’s help in everyday life, e.g. whether you will live in your own household with a caregiver or want to go to a home or to the household of children or relatives.
Should we and whom should we tell that we suffer from dementia?
After you find out your diagnosis you should share it with your closest friends and relatives, as some may be scared and withdrawn. People who cannot be part of the support circle at first can join later. The roles and responsibilities of relatives and friends will change as the disease progresses. Some of the dementia patient’s primary responsibilities will be transferred to another person (family member or caregiver). It can be difficult, but adapting to change and accepting help from others can help a person with dementia remain independent for longer. Be open about your feelings. Learn to ask for help by saying what kind of support you need and how they can help you.
Family and friends are very important!
Family and friends certainly have a key role to play in supporting people with dementia, including a valuable connection to the patient’s past. The most important thing that relatives can do is to continue to support the patient and encourage him to remain an active member of the family and local community.
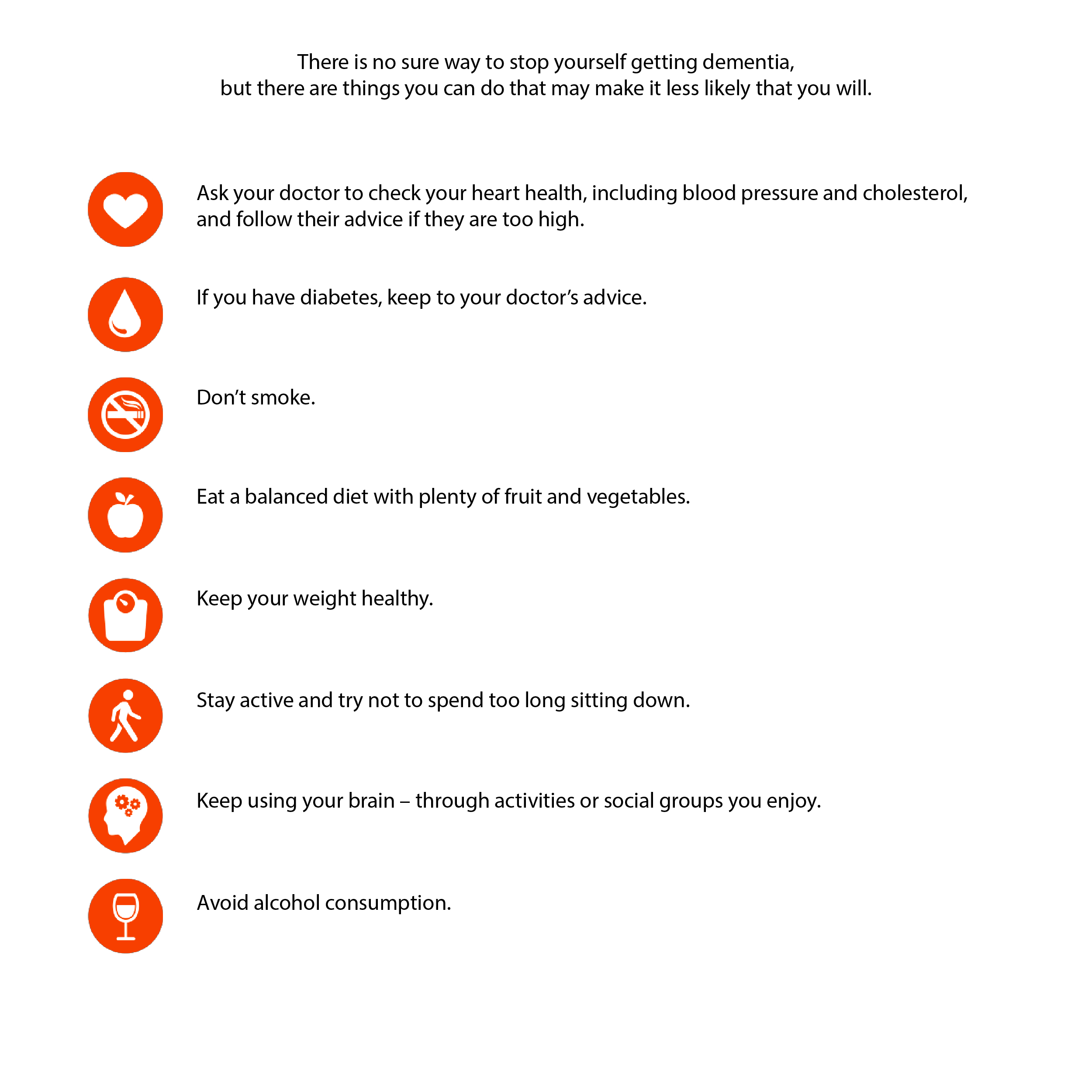
Take care of your physical health: eat healthy and be active, rest when you are tired. Visit your doctor of choice regularly. Engage in mentally stimulating activities: read, do crossword puzzles, try a new hobby. Talk to friends. Stay socially engaged. Actions that you once did easily will become increasingly difficult. Accepting change and learning coping skills can lead to the establishment of a new system of balance and stress reduction.
Practical recommendations for people in the immediate vicinity:
- First of all, it is necessary to provide an environment without potential dangers for the patient, preferably without moving to a new, unfamiliar environment. Arrange the space with as little furniture as possible, arranged so as not to obstruct safe passage and movement. Replace potentially slippery surfaces with textile pads, regulate showers with automatic thermometers, adjust lighting, keep medicines, chemicals, tobacco and alcohol off-limits;
- Get informed about the disease;
- Avoid criticizing behavior and avoid conflicts with a person affected by dementia;
- Clearly structure daily activities and establish a routine (getting up at the same time, meals, therapy, maintaining hygiene);
- Show respect to the patient, include him in decision-making, be considerate, reasonable and gentle in communication and
- In the late stages, provide the patient with a bracelet with basic information (name, surname, address, phone number of the contact person).
A diagnosis of dementia does not mean the end of life. With appropriate family and community support, adequate treatment and recommendations for organizing living conditions at home, in the home and in the hospital, we can provide dementia patients with a better quality and more fulfilling life.
Our efforts, as those responsible on behalf of the profession, are directed against loneliness and isolation, and towards preserving dignity and independence within the full limits of (growing) possibilities.